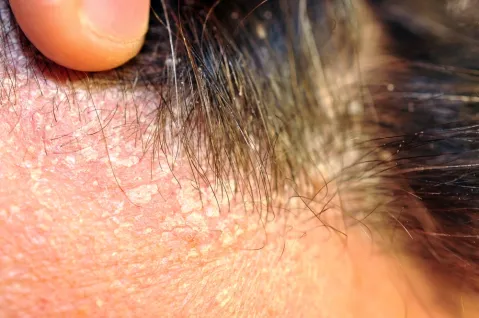
Seborrheic dermatitis (SD) is a chronic, relapsing inflammatory skin disorder characterized by erythematous, scaly lesions affecting areas rich in sebaceous glands, most commonly the scalp, face, and upper trunk. Driven by an abnormal immune response to Malassezia species, SD represents a spectrum from mild dandruff to severe facial or truncal involvement, often fluctuating with environmental and systemic factors, such as stress, weather changes, and immunosuppression.
Prevalent in 2% to 5% of adults, with higher incidence in men and individuals with neurologic or immunocompromising conditions, SD remains one of the most frequent conditions encountered in dermatologic practice. Optimal management requires understanding its multifactorial pathogenesis, evidence-based topical and systemic therapies, and strategies for long-term maintenance to reduce recurrence.
This factsheet summarizes key insights for clinicians on presentation, diagnosis, epidemiology, and treatment options, offering a concise, evidence-based reference for daily dermatologic care.
Seborrheic Dermatitis Factsheet
|
|
|
|
Presenting Symptoms |
|
|
Affected Demographics |
|
|
Diagnosis |
|
|
Treatment Options |
|
References
- Adalsteinsson J, Kaushnik S, Muzumdar S, Guttman-Yassky E, Ungar J. An update on the microbiology, immunology and genetics of seborrheic dermatitis. Exp Dermatol. 2020;29(5):481-489. doi:10.1111/exd.14091
- Navarro Triviño FJ, Velasco Amador JP, Rivera Ruiz I. Seborrheic dermatitis revisited: pathophysiology, diagnosis, and emerging therapies—a narrative review. Biomedicines. 2025;13(10):2458. doi:10.3390/biomedicines13102458
- Turchin I, Albrecht L, Hanna S, et al. Current understanding of seborrheic dermatitis: epidemiology, burden of disease, and pathophysiology. J Cutan Med Surg. 2025;12034754251368840. doi:10.1177/12034754251368840
- Piérard-Franchimont C, Goffin V, Decroix J, Piérard GE. A multicenter randomized trial of ketoconazole 2% and zinc pyrithione 1% shampoos in severe dandruff/seborrheic dermatitis. Skin Pharmacol Appl Skin Physiol. 2002;15(6):434-441. doi:10.1159/000066452
- Papp KA, Papp A, Dahmer B, Clark CS. Single-blind, randomized controlled trial evaluating the treatment of facial seborrheic dermatitis with hydrocortisone 1% ointment compared with tacrolimus 0.1% ointment in adults. J Am Acad Dermatol. 2012;67(1):e11-e15. doi:10.1016/j.jaad.2011.02.032
- Gupta AK, De Doncker P, Talukder M. Role of topical ketoconazole in therapeutic hair care beyond seborrheic dermatitis and dandruff. JEADV Clinical Practice. 2025;4(4):710-718. doi:10.1002/jvc2.70026
- Gupta AK, Versteeg SG. Topical treatment of facial seborrheic dermatitis: a systematic review. Am J Clin Dermatol. 2017;18(2):193-213. doi:10.1007/s40257-016-0232-2
- Ghodsi SZ, Abbas Z, Abedeni R. Efficacy of oral itraconazole in the treatment and relapse prevention of moderate to severe seborrheic dermatitis: a randomized, placebo-controlled trial. Am J Clin Dermatol. 2015;16(5):431-437. doi:10.1007/s40257-015-0133-9
- Okokon EO, Verbeek JH, Ruotsalainen JH, Ojo OA, Bakhoya VN. Topical antifungals for seborrhoeic dermatitis. Cochrane Database Syst Rev. 2015;(5):CD008138. doi:10.1002/14651858.CD008138.pub3